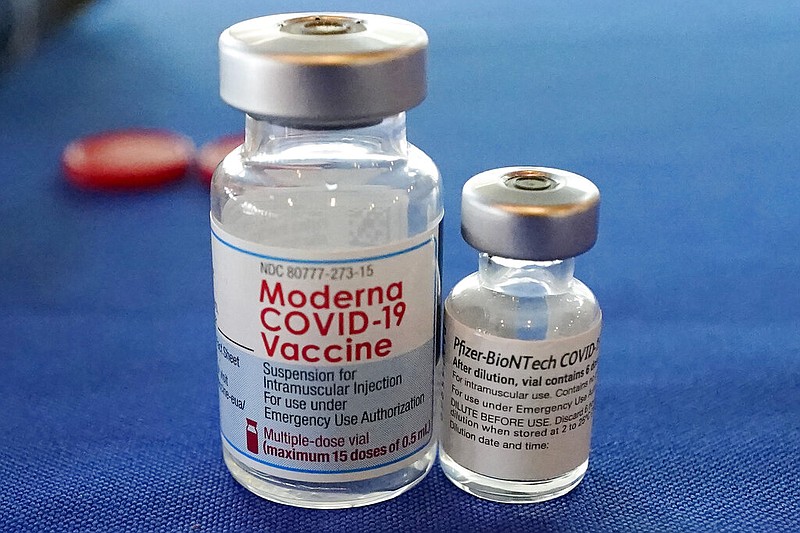
LOS ANGELES -- With coronavirus cases increasingly on the upswing across the nation, an updated covid-19 vaccine is likely to come out even earlier than expected.
Coronavirus transmission has been rising this summer, and hospitalizations, while still low, have recently started to tick up as well. As they do, officials are closely watching another subvariant that has raised more questions: BA.2.86, nicknamed Pirola, after an asteroid.
Nationally, there were 12,613 weekly covid-19 hospitalizations for the week that ended Aug. 12 -- double the number from the start of this summer, but just one-third of the level seen at this time last year.
The U.S. Food and Drug Administration said this year's updated version of the covid-19 vaccine is likely to come out by the middle of next month, a bit earlier than the late September timeline previously announced by the Department of Health and Human Services.
The earlier-than-expected arrival became apparent after the U.S. Centers for Disease Control and Prevention scheduled a Sept. 12 meeting of its Advisory Committee on Immunization Practices, a likely indication that the vaccine would become available shortly afterward.
The latest version of the vaccine is designed against the omicron subvariant XBB.1.5, unofficially known as Kraken. Unlike last year's formulation, a bivalent vaccine that was designed against the ancestral coronavirus strain and the BA.5/BA.4 omicron subvariants that were circulating at the time, the upcoming vaccine will be monovalent, specifically designed against XBB.1.5.
Kraken, dominant as of this spring, has seen other upstart subvariants rise to compete against it, such as XBB.1.16 (unofficially refered to as Arcturus) and EG.5 (also known as Eris). The differences between these subvariants are relatively minor, and it's expected that the new vaccine will be effective against all three.
PURSUING PIROLA
In a CDC risk assessment, the agency said Pirola "may be more capable of causing infection in people who have previously had covid-19 or who have received covid-19 vaccines."
While only about a dozen cases of the new BA.2.86 variant have been reported worldwide -- including three in the United States -- experts say this variant requires intense monitoring and vigilance that many of its predecessors did not. That's because it has even greater potential to escape the antibodies that protect people from getting sick, even for those who have recently been infected or vaccinated.
The latest variant does not appear to make people sicker than earlier iterations of the virus; antiviral treatments should still work against it and tests should still detect it, according to the risk assessment.
The effectiveness of the upcoming vaccine against Pirola is still being evaluated, the CDC said Wednesday, but the agency still expects that the new version will be effective at reducing severe disease and hospitalization.
"At this point, there is no evidence that this variant is causing more severe illness. That assessment may change as additional scientific data are developed," the agency added.
Unlike more recently identified subvariants, which might have one or two mutations that distinguish them from earlier versions, Pirola has 36 distinct mutations from XBB.1.5, "which is making people raise their eyebrows," said Dr. Peter Chin-Hong, a UC San Francisco infectious disease expert.
"BA.2.86," he said, "is so different that people worry that the vaccine in the fall won't be a perfect match -- but nevertheless, it will still protect people against serious disease."
"And who knows if it's even going to become ruler of the roost? It really hasn't taken off so far that we know," Chin-Hong added. "But again, sequencing always lags and not a ton of people are doing sequencing any more around the world."
Very few cases of Pirola have been identified in the United States thus far. But in some parts of Europe, Pirola now makes up perhaps 1% to 2% of cases, and the fact that it's on more than one continent suggests it is spreading, Chin-Hong said.
GAINING NOTICE
On Aug. 12, virologists in Israel were the first to announce that BA.2.86 had been detected in a patient. Scientists in Denmark, Britain, South Africa, Switzerland and Thailand soon followed. Some of the samples were collected in late July. The sporadic reports add up to evidence of international transmission, but the magnitude is unclear.
In one Swiss town, roughly 2% of coronavirus particles sequenced in a wastewater sample taken in early August were BA.2.86 variants. That was the first sign of a variant spreading within a community.
"Finding BA.2.86 in yet an additional country -- now in wastewater rather than a patient -- is another piece of evidence that BA.2.86 is globally widespread by now," Tanja Stadler, a professor at the Swiss Federal Institute of Technology who announced the findings, wrote in an email. "It is still too early to tell if this variant will cause a major wave."
The United States is experiencing an uptick of cases believed to be driven primarily by XBB and the new EG.5 variant, but several BA.2.86 cases have been announced in the past week. One of the BA.2.86 cases was discovered in Michigan in an older adult who was not hospitalized, while another was detected in a traveler arriving at Dulles International Airport in Virginia. A third case was detected in an Ohio wastewater sample.
Areas where BA.2.86 has been detected have not seen disproportionate increases in hospitalizations, the CDC said, suggesting it's not more likely to cause more severe illness than other omicron subvariants.
Still, those infected with the Pirola subvariant have so far experienced generally mild symptoms, Chin-Hong said. Based on what's currently known, if Pirola does become dominant, "at some point, it may fuel another round of transmission, and may find people who are 'no-vids"' -- people who have never been infected -- "or people who are more vulnerable to getting ill," Chin-Hong said.
Regardless of the new mutations in Pirola, Chin-Hong said, the anti-covid therapeutic drugs Paxlovid and remdesivir should remain effective.
Generally speaking, Chin-Hong said many people who have been infected with the coronavirus this summer did not require hospitalization, likely because they were vaccinated, had been previously infected or both. Even those covid-19 patients who have been hospitalized, Chin-Hong said, are generally requiring shorter stays than earlier in the pandemic.
Still, those who are being hospitalized tend to be older and those who haven't received a covid-19 booster shot in the past year -- meaning they are not considered "up to date."
Areas of the country that are seeing particularly notable increases in new weekly covid-19 hospitalizations are in the South, CDC data show. In a blog post, Dr. Eric Topol, director of the Scripps Research Translational Institute in San Diego, said recent trends underscore how "the pandemic isn't over."
Topol described the recent increase in transmission as a "wavelet" that could pick up steam but is more likely related to waning immunity and behavior than the latest subvariants.
"The fact that the inexorable evolution of the virus continues -- to find new hosts and repeat hosts -- cannot be ignored," he wrote.
"At the moment there's no reason for alarm. ... What we'll see in the weeks ahead is whether BA.2.86 takes hold or not. If it does, that will pose a new challenge, and make the 'updated' booster shots considerably less helpful than what was conceived when XBB.1.5 was selected as the target," Topol wrote.
WHAT ARE THE ODDS?
The biggest unknown is whether the BA.2.86 will be transmissible enough to cause a surge. A variant adept at evading immunity would not take off in a population if it does not spread efficiently and multiply.
"It is still a possibility we either see this variant spread very widely as happened with the original omicron," said Jesse Bloom, a computational biologist who monitors coronavirus variants at the Fred Hutchinson Cancer Center in Seattle, "or it doesn't end up spreading very widely and we continue to have these XBB variants."
Experts have paid close attention to Bloom's analysis of BA.2.86, which stressed that the evolutionary jump is on par with the one that gave rise to omicron.
Officials say they should have a clearer understanding of the variant's transmissibility in the coming weeks as surveillance ramps up in response to the threat.
In the United States, the CDC no longer offers variant estimates for most regions of the country because of declines in surveillance.
Variant watchers say they're worried the world may be blind to the true reach of BA.2.86 as a result.
"The situation served as a significant wake-up call," said Rajendram Rajnarayanan, a computational biologist who monitors genetic-sequencing data as part of an international consortium of virus watchers, in an email. "This is especially true as global testing and sequencing infrastructure started disappearing (or is in the process of getting dismantled) following the end of pandemic declarations earlier this year."
Information for this article was contributed by Rong-Gong Lin II of the Los Angeles Times(TNS) and by Fenit Nirappil of The Washington Post.