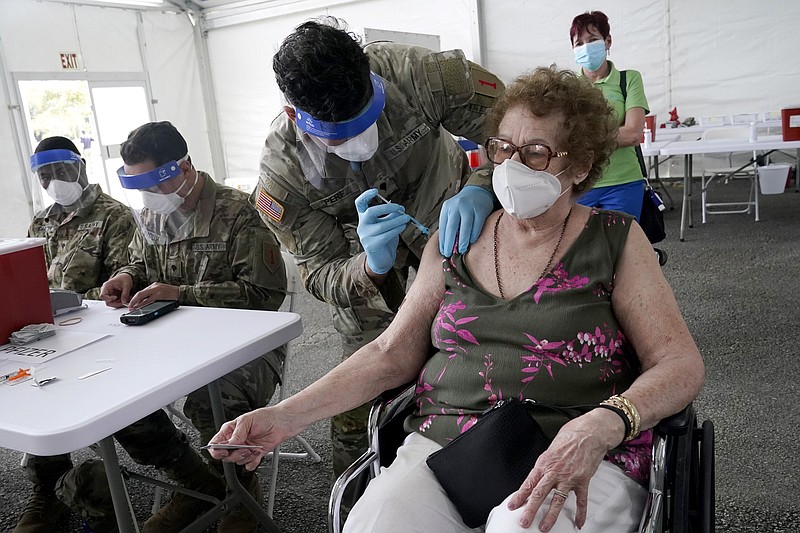
PORTLAND, Ore. -- Jean Andrade, an 88-year-old who lives alone, has been waiting for her covid-19 vaccine since she became eligible under state guidelines nearly a month ago. She assumed her caseworker would contact her about getting one, especially after she spent nearly two days stuck in an electric recliner during a recent power failure.
It was only after she saw a TV news report about competition for the limited supply of shots in Portland, Ore., that she realized no one was scheduling her dose. A grocery delivery service for homebound older people eventually provided a flyer with vaccine information, and Andrade asked a helper who comes by for four hours a week to try to snag her an appointment.
"I thought it would be a priority when you're 88 years old and that someone would inform me," said Andrade, who has lived in the same house for 40 years and has no family members able to assist her. "You ask anybody else who's 88, 89, and don't have anybody to help them, ask them what to do. Well, I've still got my brain, thank God. But I am very angry."
Older adults have top priority in covid-19 immunization drives the world over right now, and hundreds of thousands of them are spending hours online, enlisting their children's help and traveling hours to far-flung pharmacies in a desperate bid to secure a vaccine. But an untold number like Andrade are getting left behind, unseen, because they are too overwhelmed, too frail or too poor to fend for themselves.
[CORONAVIRUS: Click here for our complete coverage » arkansasonline.com/coronavirus]
The urgency of reaching this vulnerable population before the nation's focus turns elsewhere is growing as more Americans in other age and priority groups become eligible. With the clock ticking and many states extending shots to people as young as 55, nonprofits, churches and advocacy groups are scrambling to find isolated elders and get them inoculated before they have to compete with an even bigger pool -- and are potentially forgotten about as vaccination campaigns move on.
An extreme imbalance between vaccine supply and demand in almost every part of the United States makes securing a shot a gamble. In Oregon, Andrade is vying with as many as 750,000 residents 65 and older, and demand is so high that appointments for the weekly allotment of doses in Portland are snapped up in less than an hour. On Monday, the city's inundated vaccine information call line shut down by 9 a.m., and online booking sites have crashed.
Amid such frenzy, the vaccine rollout there and elsewhere has strongly favored healthier seniors with resources "who are able to jump in their car at a moment's notice and drive two hours" while more vulnerable older adults are overlooked, said James Stowe, director of aging and adult services for an association of city and county governments in the Kansas City area.
"Why weren't they the thrust of our efforts, the very core of what we wanted to do? Why didn't it include this group from the very outset?" he said of the most vulnerable seniors.
Some of the older adults who have not received vaccines yet are so disconnected they don't even know they are eligible. Others realize they qualify, but without internet service and often email accounts, they don't know how to make an appointment and can't get to one anyway -- so they haven't tried.
Still others have debilitating health issues that make leaving home an insurmountable task, or they are so terrified of exposure to the virus that they'd rather go unvaccinated than risk venturing out in public to get a shot.
In Kansas City, Mo., 75-year-old Pat Brown knows she needs the vaccine because her asthma and diabetes put her at higher risk of serious covid-19 complications. But she hasn't attempted to schedule an appointment and didn't even know if they were being offered in her area yet; she says she is too overwhelmed.
"I don't have no car, and it's hard for me to get around places. I just don't like to go to clinics and have to wait because you have to wait so long," Brown said, adding that she is in constant pain because of spinal arthritis. "I couldn't do it. My back would give out ... and I don't have the money to take a cab."
The pandemic has also closed senior centers, libraries and churches -- all places where older Americans might remain visible in their communities and get information about the vaccine. And some public health departments at first relied on mass emails and text messages to alert residents they were eligible, thereby missing huge chunks of the senior population.
"Do you think everyone has internet access? Do you really think everyone has email?" said Denise LaBuda, spokeswoman for the Council on Aging of Central Oregon. "We just don't know where they all are. They have to raise their hand -- and how do they raise their hand?"
INSURERS HELPING
To counter access disparities, the Biden administration said Wednesday that it will partner with health insurance companies to help vulnerable older people get vaccinated. The goal is to get 2 million of the most at-risk seniors vaccinated soon, White House coronavirus special adviser Andy Slavitt said.
He said insurers will use their networks to contact Medicare recipients with information about vaccines, answer questions, find and schedule appointments for first and second doses and coordinate transportation. The focus will be on reaching people in medically underserved areas.
Nonprofits, churches and advocates for older people have already spent weeks figuring out how to reach disadvantaged Americans older than 65 through a patchwork and grassroots effort that varies widely by location.
Some are partnering with charities like Meals on Wheels to distribute vaccine information or grocery-delivery programs like the one that alerted Andrade. Others are mining library card rosters, senior center membership lists and voter registration databases to find disconnected older people.
Reaching out through organizations and faith groups that marginalized older Americans already trust is key, said Margaret Scharle, who developed a vaccine outreach toolkit for her Catholic parish in Oregon. The "low-tech" approach, which other charities started using, relies on door-knocking, paper brochures and scripted phone calls to communicate with older residents.
"Once you've been blocked so many times in trying to make an appointment, you might give up. So we are working as hard as we can to penetrate the most marginalized communities, to activate networks that are already existing," said Scharle.
In Georgetown, S.C., a rural community where many of the 10,000 residents are the descendants of slaves, the local NAACP chapter is using its rolls from a November get-out-the-vote drive to get the oldest citizens out for the vaccine. Chapter President Marvin Neal said they are trying to reach 2,700 people to let them know they are eligible for a shot and to offer help booking appointments.
Many of those individuals don't have internet service or transportation, or suffer from medical issues like dementia, he said.
"Some are not even aware that the vaccine is even in their community, that's the challenge," Neal said. "It's like they're just throwing up their hands in the air and hoping somebody steps in. Because all the ones I have talked to want the vaccine. I haven't had one yet that didn't say, 'Sign me up.'"
2 MILLION SHOTS
Meanwhile, the average number of vaccine doses being administered across the United States per day topped 2 million for the first time Wednesday, according to data from the Centers for Disease Control and Prevention. A month ago, the average was about 1.3 million.
President Joe Biden set a goal of administering more than 1.5 million doses a day, which the nation has now comfortably exceeded.
Biden has also promised to administer 100 million vaccines by his 100th day in office, which is April 30. As of Thursday, 54 million people have received at least one dose of a covid-19 vaccine. Johnson & Johnson's one-shot vaccine was authorized for emergency use Saturday, but those doses do not appear yet in the CDC data.
And Biden has made equity a major focus of his pandemic response, saying he wants pharmacies, mobile vaccination units and community clinics that help underserved communities to help increase the pace of vaccinations.
Experts say Black and Hispanic Americans are being vaccinated at lower rates because they face obstacles such as language barriers and inadequate access to digital technology, medical facilities and transportation. But mistrust in government officials and doctors also plays a role and is fed by misinformation that is spread on social media. In cities across the country, wealthy white residents are lining up to be vaccinated in low-income Hispanic and Black communities.
Biden said Tuesday that the country would have enough doses available for every U.S. adult by the end of May, although he said it would take longer to inoculate everyone and he urged people to remain vigilant by wearing masks.
TESTING FALLS
The average number of tests being conducted every day in America has plummeted by 33.6% since January, according to the Covid Tracking Project.
That statistic that has many experts deeply concerned because it comes just as America's recent decrease in infections and deaths is stalling at a worrisome high level. Testing is a key tool to stopping coronavirus transmission; without it, the virus has the potential to spread unchecked.
Some of those declines can be attributed to the overall improvement of the pandemic in America. With decreased cases and less transmission, fewer people have been experiencing symptoms. But there are other factors at play as the U.S. pandemic drags on: Getting tested is time-consuming. Some people also do not want to isolate or miss work because of a pending or positive test, according to testing coordinators and experts.
Only a small fraction of the U.S. population -- about 54 million people -- has been vaccinated. Until more people receive their shots, testing remains one of the country's main tools for stopping the chain of transmission.
At the same time, more-transmissible variants of the virus are spreading and officials are repealing restrictions, making a spring resurgence of the virus possible.
Testing coordinators in multiple states said they are seeing a growing reluctance to get tested. Many people worry that the recent emphasis on how vaccines will eventually end the pandemic have caused people to discount the danger still present.
Some health departments -- already underfunded and overworked -- are struggling to maintain testing sites even as they try to scale up vaccinations.
Information for this article was contributed by Gillian Flaccus, Heather Hollingsworth, Russ Bynum and Sara Cline of The Associated Press; by Ruth Graham of The New York Times; and by William Wan of The Washington Post.